
Laszlo Z, Rössler A, Hinghofer-Szalkay H

Laszlo
Z, Rössler A, Hinghofer-Szalkay H
Cardiovascular changes during and after different LBNP levels in men
Aviat Space Environ Med 1998; 69:32-9
![]()
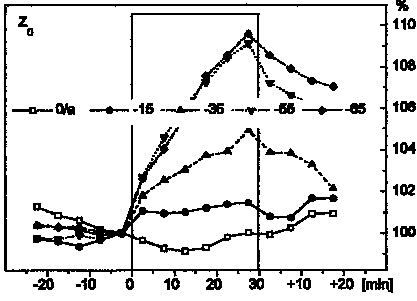
Time course
of basic thoracic bioimpedance during different
levels of LBNP >>
Background & methods: This study quantifies
hemodynamic and thoracic impedance (TI) changes with four levels
of lower body negative pressure (LBNP) from -15 to -65 mm Hg in 7
healthy men in supine position 20 min before (pre-LBNP), 30 min
during, and 20 min after suction (post-LBNP) as well as without
suction (LBNP-0, rest control).
Results: LBNP >15mmHg increased basic TI by up to 2.2 Ohms (+9.5%). TI-computed stroke volume index (SVI) continuously decreased with time up to -12%, -28%, -36%, and -40% at the end of LBNP-15, -35, -55, and -65. TI-computed cardiac index decreased most (-14%) at LBNP-15 and -35, resulting in a 19% increase of calculated total peripheral resistance index at those intensities. Mean arterial pressure (MAP) did not change in any systematic way with lower LBNP levels, but increased +4.7% and +7.4% at the end of LBNP-55 and -65, respectively. Heart rate (HR) remained unchanged at LBNP-15, but continuously increased to reach +22%, +42%, and +55% at the end of LBNP-35, -55, and -65. After finishing LBNP, HR fell to values below both pre-LBNP and rest control for 5 min (“post-LBNP bradycardia”). SVI transiently returned to, and MAP increased above, pre-LBNP levels after suction.
Conclusion: Different levels of lower body subatmospheric pressure produced quantitatively different time course and dose-response patterns and remained non-hypotensive up to -65 mm Hg suction. In this study, heart rate was depressed after LBNP (“post-LBNP bradycardia”), while arterial blood pressure and TI-computed total peripheral resistance exceeded control levels with LBNP35.
Interpretation: The findings indicate an altered cardiovascular state after 30 min of simulated orthostasis. Higher LBNP intensity seems to evoke additional responses which aid to stabilize venous return, cardiac output, and perfusion.
![]()